 Class IA drugs slow SA node automaticity and increase AV node conduction time and refractoriness, but antimuscarinic actions (especially for quinidine and disopyramide) oppose these effects. Because onset of block is rapid and because cardiac electrophysiologic (EP) effects are more pronounced at fast rates (use-dependence), class IA drugs are effective for suppressing reentrant atrial and ventricular dysrhythmias. 
Therefore, class IA drugs slow conduction, prolong action potential duration and repolarization, and increase effective refractoriness of atrial and ventricular myocardium. 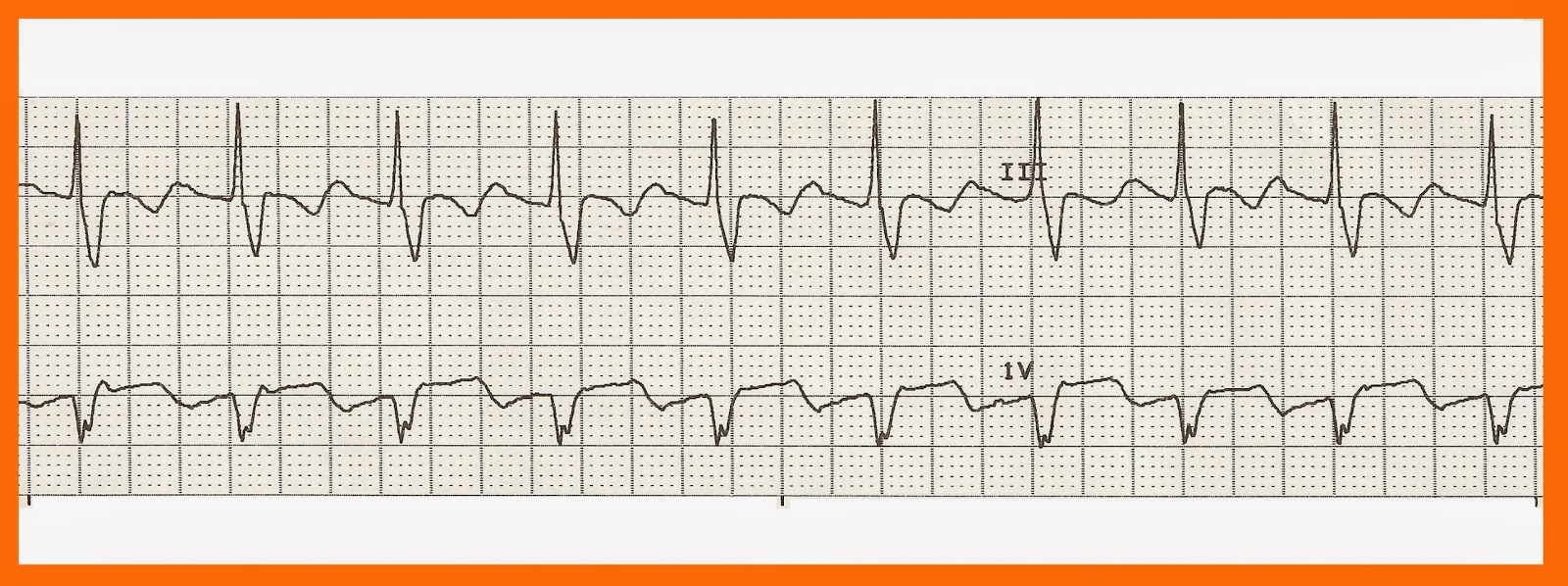
They also (especially quinidine) block K sup + repolarization currents (a class III action). Vaughan Williams class IA drugs (quinidine, procainamide, disopyramide) primarily block open Na sup + channels with intermediate time constants for recovery from block (300–1500 ms). In contrast, with abnormal ventricular activation, the QRS complex has about an equal likelihood of having right or left bundle branch block morphology. Aberration caused by the Asmann phenomenon occurs because refractoriness is longer after the long cycle beat, so that the subsequent short cycle beat propagates, whereas the distal conducting system is still partially refractory. Also, QRS aberration is more likely with slow heart rates or when a short cycle beat follows a long cycle beat in patients with atrial fibrillation (Ashman phenomenon Figure 3). For example, the higher incidence of right versus left bundle branch block pattern QRS aberration with premature supraventricular beats or tachycardia (SVT) is explained by longer refractoriness of the right bundle branch. QRS aberration has many possible causes, all of which are explained by differential or altered refractoriness of the ventricular specialized conducting tissues. The term QRS aberration does not apply to fixed ventricular conduction defects (i.e., fascicular or bundle branch block). Aberrant beats are easily misdiagnosed and mismanaged as ventricular dysrhythmias. Widened (> 0.10 s) or bizarre QRS complexes result from abnormal ventricular conduction of supraventricular beats (ventricular aberration) or abnormal ventricular activation with ventricular beats. Comparable data are not available for patients in postanesthetic or surgical intensive care units. 
Severe adverse outcomes, defined as need for significant management (i.e., antidysrhythmic drugs, electrical devices, or cardiopulmonary resuscitation) with or without chronic disability or death resulting from dysrhythmias, occurred in 1.6% of these patients. Most patients (90.7%) were American Society of Anesthesiologists (ASA) physical status 1 and 2. The Multicenter Study of General Anesthesia reported a 70.2% incidence of tachycardia, bradycardia, or dysrhythmias in 17,201 patients having general anesthesia for a variety of surgical procedures. Incidences greater than 90% are possible with continuous monitoring in patients having cardiothoracic surgery. only potentially dangerous ones), continuous surveillance versus casual observation, patient characteristics, and the nature of surgery. 
The incidence of intraoperative dysrhythmias depends on the definition (e.g., any dysrhythmia vs. Advances in diagnosis and management of dysrhythmias since 1970 include 1) elucidation of mechanisms for most clinical dysrhythmias, with application of this knowledge to more effective preventive, remedial, and specific management with drugs or devices (pacemakers, cardioversion) 2) availability of new drugs for intravenous use, including adenosine, amiodarone, bretylium, diltiazem, esmolol, ibutilide, and verapamil 3) recognition of the potential for lethal ventricular prodysrhythmia with antidysrhythmic drugs 4) technologic advances with noninvasive transcutaneous and transesophageal pacing and 5) use of surgical or catheter ablation of dysrhythmic foci or reentrant pathways for management of atrial and ventricular tachydysrhythmias. Cardiac electrophysiology and mechanisms for perioperative dysrhythmias were reviewed in the journal by Atlee and Bosnjak in 1990. Since a review by Katz and Bigger in 1970, no discourse on recognition and management of perioperative cardiac dysrhythmias has appeared in Anesthesiology, despite important advances in diagnosis and treatment. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
